
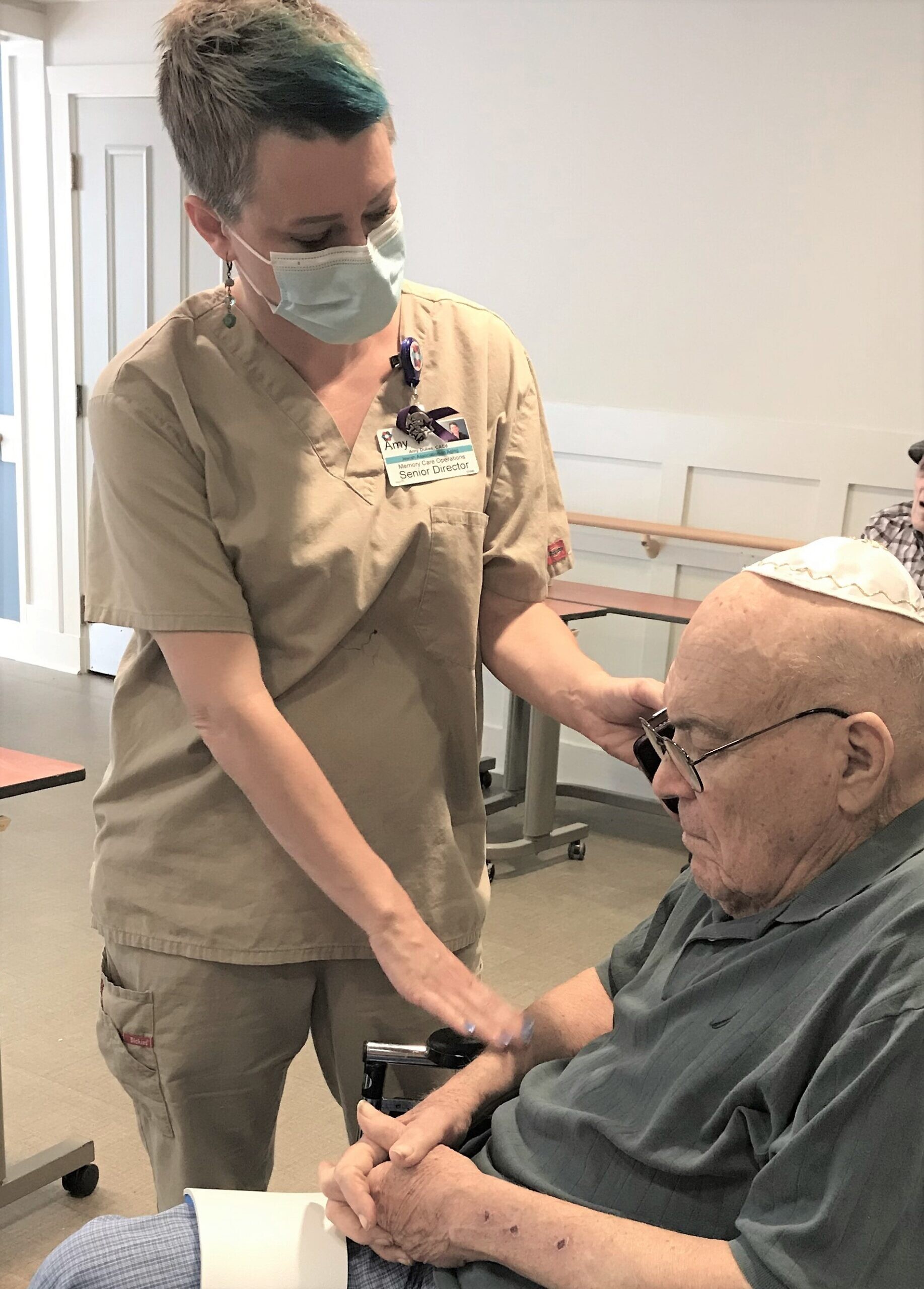
A family visits an elderly resident at a senior facility run by the Jewish Association on Aging in Pittsburgh. Credit: Courtesy.
Nursing-home administrators keep up the battle against the coronavirus, as they work to improve their in-house responses and close care of patients.
As America’s battle with the novel coronavirus has raged America’s Jewish community has suffered its share of losses, particularly early on when COVID-19 swept through the boroughs of New York City and Upstate New York. No age group has been as widely affected as the elderly, making nursing homes, assisted-living facilities and senior residences ground zero in the battle against the virus, at least at first.
While other states in the Northeast—Massachusetts, Connecticut, New Jersey and Pennsylvania—were also hit hard at the beginning of the pandemic in March and April, cases of infection lessened significantly after months of social distancing and lockdowns. Once thought that the virus would subside as the weather warmed in late spring and summer, that did not happen, and now, swaths of the U.S. South are seeing daily infection rates that rival the worst days in New York City.
Florida, Texas, Arizona, Louisiana and Georgia are facing a massive surge in new infections, hospitalizations and deaths. Given these ongoing statistics, what can be learned from early hot spots to help states now facing a similar crisis?
JNS spoke with Jewish nursing-home administrators in Miami, Pittsburgh and New York to hear from those on the front lines about how they have coped and are still coping, in addition to the lessons learned and efforts to protect the elderly going forward.
One decision they noted was a March 25 mandate by the New York State Department of Health requiring nursing homes to accept coronavirus patients considered to be “medically stable” after being discharged from a hospital, unless facilities could demonstrate that they were unprepared to do so. The order did not require these patients to be tested for COVID-19; in fact, it explicitly said not to.
Gov. Andrew Cuomo later rescinded the order, but not before much damage was done, with the virus spreading rapidly among the elderly. States have learned much since then, particularly New York, which flattened its curve before the summer started.
The Centers for Disease Control and Prevention also listed guidelines including mask-wearing, social distancing and hand-washing/hygiene care. It also reported, as of July 13, a total of 3,296,599 cases of COVID-19 with 134,884 related deaths in the United States
(Statistics below from Worldometers.info, dated 7/13/2020)
Miami (Florida)
Governor: Ron DeSantis (R-Fla.)
Statewide Mask Mandate: Not required
Cases Citywide (Miami-Dade County): 67,712
Cases Statewide: 282,000
Deaths Citywide: 1,143
Deaths Statewide: 4,276
Height of Cases: July 12 (15,000 new cases)
Miami Jewish Health is comprised of a 370-bed nursing home, an assisted-living facility that is home to 80, and an independent-living facility for 60. It is the largest nursing home in Southeast Florida, according to president and CEO Jeffrey Freimark.
The system has had 57 COVID-19 cases since early March, with 10 residents having died as a result of complications from the virus.
“We mourn, but the majority of the folks … have returned to their home units fully recovered and in good health … most of that return has been in recent weeks,” said Freimark.
In its assisted-living facility, two residents contracted COVID-19, and both died. Staff members have also tested positive, though no deaths ensued. No one in its independent-living facility has contracted COVID-19.
Because Miami Jewish Health is part of the state’s Program of All-Inclusive Care for the Elderly (PACE)—a nonprofit to assist seniors—its mandate includes taking patients recuperating from hospitals. And since its facilities include hospital-like wings with “the right airflow to treat COVID-19 patients,” they have accepted medically stable COVID-19 patients released from hospitals, according to Freimark.
“These units are totally isolated; there’s no herding of COVID-19-positive with anyone else,” said Freimark, adding that employees who work on these units do not interact with uninfected residents.
Communal dining has also ended as residents have been in “complete lockdown mode.”
“We closed the campus down in advance of the close order; some people were upset by that,” acknowledged Freimark. “But we have started drive-by visits” in which residents’ families can talk with loved ones from their cars at least 10 feet away.

As of June 8, they reported only one COVID-19 positive case in the facility.
Freimark said the effort to provide residents and staff with PPE has been “front of mind” from the start—masks, gowns, gloves and booties have been bought in huge quantities and reused only after being disinfected and sanitized.
“We work with the University of Miami to do the disinfecting and sanitizing,” he said. “An employee is never asked to wear the same PPE without it having gone through the disinfection process.”
With help from the Greater Miami Jewish Federation, Miami Jewish Health raised $1 million in a campaign to acquire PPE and to provide additional pay for staff in the facility’s COVID-19-positive areas.
“Nursing-home workers who are going in to deal with COVID-19 are no less heroic than any of our country’s health-care workers,” he noted.
The virus, however, is surging through the state: Florida reported 15,000 new cases on Sunday, the highest number yet in any state in a single day.
And now heading into hurricane season, Freimark is hoping for the best while preparing for the worst.
Between the tsunami of contagion from overseas, the “breakdown in the supply chain” for PPE, and the March 25 mandate, he feels his counterparts in New York got hit with a “perfect storm” in the spring.
But now, he and his colleagues are at the center of the storm.
“We could find ourselves at the crossroads of a hurricane and a COVID-19 environment with the supply chain again an issue,” he cautioned, “and that would certainly be a challenge.”
Pittsburgh (Pennsylvania)
Governor: Tom Wolf (D-Pa.)
Statewide Mask Mandate: Required
Cases Citywide (Allegheny County): 5,033
Cases Statewide: 100,000
Deaths Citywide: 198
Deaths Statewide: 6,955
Height of Cases: April/May, but now seeing a slight resurgence
Far to the north and on the flip side of the equation, Pittsburgh hasn’t reported a single resident contracting COVID-19 in its Jewish nursing homes or Jewish-agency-run residential facilities to date.
“We have worked very hard to protect our elderly, and we recognize that we have been very lucky also,” said Debbie Winn-Horvitz, president and CEO of the Jewish Association on Aging (JAA), which administers several residential facilities, as well as home and community-based services in Pittsburgh.
Luck, however, was not the only thing involved.
The JAA serves a total of 4,000 seniors, including residents of Weinberg Terrace, Weinberg Village, Riverview Towers, the Charles Morris Nursing & Rehabilitation Center and the Ahava Memory Care Residence, an assisted-living facility. This spring, three JAA staff members came down with COVID-19, but it did not spread to residents.

With help from United Jewish Federation of Pittsburgh and other Jewish organizations, Winn-Horvitz’s staff has been able to procure PPE, and she believes this has made a real difference.
Pittsburgh’s JAA facilities have “hundreds of protocols in place” regulating cleaning, staff/patient interactions and PPE, said Winn-Horvitz. All staff members are required to wear N-95 masks, gowns and gloves, and change them immediately after leaving an individual’s room. Direct patient-care workers “also wear face shields.” PPE is not reused.
The first staffer who came down with COVID-19 is a “direct patient-care worker,” said Winn-Horvitz. She reported not feeling well, was sent home immediately, and after receiving a positive test stayed home until she recovered and tested negative. She has since returned to work.
As of July 13, three JAA employees have tested positive—the first on April 26, the others on July 2 and July 8, consistent with the recent spike of the coronavirus in Western Pennsylvania. As of July 13, no elderly residents have come down with the disease, according to Tinsy Labrie, director of marketing and public relations for Pittsburgh’s JAA.
Other staff protocols at Pittsburgh’s JAA facilities include “strictly changing PPE from room to room, changing out of street clothes and into scrubs when they come in to work,” and multiple separate break areas for staff working with different populations, “so that if, God forbid, it were to break out in one area, we don’t want it to spread,” said Winn-Horvitz.
Communal dining has been suspended for months. Staff members do, however, help residents participate in modified social activities from their rooms.
“They play ‘rolling Bingo,’ where one person at the end of the hall calls out the numbers to them in their rooms,” she described. Other activities include exercise classes from the doorways of their rooms, as well as recent dress-up and singalong from their doorways for the home opener of the Pittsburgh Pirates. There is also some limited visiting with family through Plexiglass barriers.
In addition to Pittsburgh’s Federation, Winn-Horvitz has expressed appreciation to the Association of Jewish Aging Services (AJAS) and the Jewish Federations of North America for helping to secure supplies.
Winn-Horvitz said she was grateful that she didn’t have to contend with an order to accept COVID-19-infected hospital patients in homes with other elderly residents as her counterparts in New York did early on when the coronavirus overwhelmed the city.
“I disagreed with Cuomo’s decision,” said Winn-Horvitz. “Not every facility was prepared” to handle that.
As cases spike in Pittsburgh’s Allegheny County, Winn-Horvitz said she is working to obtain resources to meet the state’s requirement that all nursing-home staff and residents be tested for COVID-19 by July 26.
She added, “I don’t take anything for granted because we could be next,” as Western Pennsylvania has begun to experience another spike. Nonetheless, she says “all our residents remain COVID-19 free, and we are trying to keep it that way.”
New York City (New York)
Governor: Andrew Cuomo (D-N.Y.)
Statewide Mask Mandate: Required
Cases Citywide: 224,000
Cases Statewide: 407,000
Deaths Citywide: 22,795
Deaths Statewide: 32,075
Height of Cases: March and April
According to figures released in a report this week by state health officials, some 6,500 nursing-home residents have died of COVID-19 out of a total 100,000 nursing-home residents in the state’s 613 facilities. Jewish institutions have not escaped significant loss.
Stuart Almer, chief executive of Gurwin Healthcare Systems in Commack, N.Y., a 460-bed nursing home with other facilities, explained that it stocked up on Personal Protective Equipment (PPE) and created an “isolation unit” in February in anticipation of coronavirus cases.
“We knew [similar infections] had happened in Seattle, so my instruction was, ‘Let’s get as many masks, gowns and gloves as we can,’ ” recalled Almer. The home also purchased Plexiglass panels to create the COVID-19 isolation unit.

As of March 25, when New York State’s health department under Gov. Andrew Cuomo ordered nursing homes to admit COVID-19-infected elderly from hospitals, Gurwin had one COVID-19 infected resident.
Since then, 60 Gurwin residents have died from COVID-19 in its nursing home, and 13 have died in its assisted-living facility. In the nursing home, 150 residents have recovered, and the facility has now reported zero cases of COVID-19.
Of 1,200 staff members, including nurses, health aides, administrators, and janitors, 130 tested positive for COVID-19, and one “beloved member of the housekeeping staff” has died, said Almer.
A disproportionate number of deaths at Gurwin took place among the “dementia population,” said Almer. Despite tremendous efforts by Gurwin’s staff, infection spread there partly because “they are more challenging to direct,” noted Almer. “Our staff did all they could … I’m very proud of them.”
At present, all staff is screened daily upon entrance with temperature checks. Additionally, Gurwin tests every employee weekly for COVID-19.
Almer is thankful to UJA-Federation of New York and the Association of Jewish Aging Services (AJAS) for helping to supplement Gurwin’s supply of PPE, and said additional support for more PPE and more testing—the costs of which he describes as “astronomical”—would “go a long way” to help ensure the facility remains COVID-19-free.
Family and friends from outside the facility have been prohibited from visiting residents “for months,” according to Almer, who in solidarity with families didn’t see his 89-year-old father, who lives in the facility, for three months.
Almer said he accepted the March 25 mandate because “we had an isolation unit, and the mandate was clear.” But he added that in the future, nursing homes need better representation in such fast-evolving situations.
In case of a future surge, vacant buildings, he said, including in nearby Suffolk County, could be secured by the state as dedicated COVID-19 treatment facilities. “There could be a [designated] COVID-positive facility in each county,” he suggested, emphasizing that discussion of the issue is not a matter of blame, but an opportunity for all parties to learn, which he noted is a Jewish value.

Dr. Jeffrey Farber, president and CEO of the New Jewish Home, a health system that includes a Mamaroneck nursing home and multiple elder-care facilities in Manhattan, the Bronx and Westchester, N.Y., stressed the importance of advances in testing to prevent a repeat of the COVID-19 spread in New York’s nursing homes.
In total, the New Jewish Home lost 58 residents due to COVID-19 with nearly 300 recovered. Two COVID-19-positive residents are fighting for their lives at present.
Farber doesn’t blame Cuomo’s March 25 order for the spread of coronavirus in New York’s nursing homes.
Citing this week’s report by the New York State Department of Health, he pointed to communal spread among New York’s population, including nursing-home workers, as a likely cause of infection.
“The latest numbers are 20 percent, and in communities with more density and reliance on public transportation, 30 or 40 percent” of New Yorkers have had exposure to the virus, “including asymptomatic disease,” he said.
To prevent another uptick in cases and deaths, as what occurred back in March and April, Farber said testing is key. Although they tested staff and residents “aggressively from the beginning,” the New Jewish Home has more recently started using “point of care” tests, which he said are more rapid and reliable than nasopharyngeal swab tests.
He suggested that facilities seek out any aid they can get to conduct as much testing as possible, including “point of care” tests.
“If you have those kinds of tests, then you can really do what we were unable to do and keep [the virus] out of the building,” advised Farber.
In addition to regular testing of staff and residents, other measures the New Jewish Home is taking to protect residents include suspending visitors for the time being.
He said his facility has “largely been on its own” paying for and securing PPE for staff, that “price gouging continues,” and that he has six employees working full-time on sourcing and procuring PPE.
All employees wear N-95 masks, gowns and gloves, but “we didn’t and don’t have anywhere near adequate PPE to discard PPE after every patient [interaction],” he acknowledged.
Instead, PPE is carefully managed so that individual workers can reuse their own N-95 masks after they sit for five days, considered more than ample time for the virus to die.
Asked what help he and others would appreciate from the Jewish community, he said that assistance in procuring and buying more PPE “would free up more employees to focus on patient care.”
He repeated that PPE—and more testing—at elder facilities remains crucial to put in place before, he cautioned, “the next wave.”


Comments